Clinical Focus ›› 2026, Vol. 41 ›› Issue (3): 212-218.doi: 10.3969/j.issn.1004-583X.2026.03.003
Previous Articles Next Articles
Antimicrobial resistance of carbapenem-resistant Klebsiella pneumoniae infection in patients with severe traumatic brain injury and construction of a nomogram model
Liao Yuning1, Zhong Meixing2, Lin Xiaofang3( )
)
- 1. Gannan Medical University, Ganzhou 341500, China
2. Department of Infection Management, First Affiliated Hospital of Gannan Medical University, Ganzhou 341000, China
3. Department of Infection Management, Nanfang Hospital Southern Medical University (Ganzhou People's Hospital), Ganzhou 341000, China
-
Received:2025-12-11Online:2026-03-20Published:2026-03-27
CLC Number:
Cite this article
Liao Yuning, Zhong Meixing, Lin Xiaofang. Antimicrobial resistance of carbapenem-resistant Klebsiella pneumoniae infection in patients with severe traumatic brain injury and construction of a nomogram model[J]. Clinical Focus, 2026, 41(3): 212-218.
share this article
Add to citation manager EndNote|Ris|BibTeX
URL: https://www.lchc.cn/EN/10.3969/j.issn.1004-583X.2026.03.003
| 抗菌药物 | 2019年9月- 2020年9月(n=9) | 2020年10月- 2021年9月(n=5) | 2021年10月- 2022年9月(n=5) | 2022年10月- 2023年9月(n=23) | 2023年10月- 2024年9月(n=53) | χ2值 | P值 | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 耐药株数 (例) | 耐药率 | 耐药株数 (例) | 耐药率 | 耐药株数 (例) | 耐药率 | 耐药株数 (例) | 耐药率 | 耐药株数 (例) | 耐药率 | |||
| 阿米卡星 | 0 | 0.00 | 4 | 80.00 | 1 | 20.00 | 18 | 78.26 | 53 | 100.00 | 60.543 | <0.01 |
| 阿莫西林克拉维酸 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 厄他培南 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 复方新诺明 | 0 | 0.00 | 0 | 0.00 | 0 | 0.00 | 22 | 95.65 | 50 | 94.34 | 66.333 | <0.01 |
| 替加环素 | 0 | 0.00 | 0 | 0.00 | 0 | 0.00 | 0 | 0.00 | 0 | 0.00 | / | / |
| 头孢曲松 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 头孢他啶 | 8 | 88.89 | 5 | 100.00 | 5 | 100.00 | 22 | 95.65 | 53 | 100.00 | 33.250 | <0.01 |
| 头孢西丁 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 头孢呋辛 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 头孢吡肟 | 7 | 77.78 | 3 | 60.00 | 3 | 60.00 | 23 | 100.00 | 53 | 100.00 | 33.048 | <0.01 |
| 头孢哌酮舒巴坦 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 亚胺培南 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 左氧氟沙星 | 2 | 22.22 | 3 | 60.00 | 3 | 60.00 | 22 | 95.65 | 53 | 100.00 | 51.482 | <0.01 |
| 哌拉西林他唑巴坦 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 头孢他啶阿维巴坦 | 0 | 0.00 | 0 | 0.00 | 0 | 0.00 | 0 | 0.00 | 0 | 0.00 | / | / |
Tab.1 Analysis of the number of CRKP-resistant strains and drug resistance (n, %)
| 抗菌药物 | 2019年9月- 2020年9月(n=9) | 2020年10月- 2021年9月(n=5) | 2021年10月- 2022年9月(n=5) | 2022年10月- 2023年9月(n=23) | 2023年10月- 2024年9月(n=53) | χ2值 | P值 | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 耐药株数 (例) | 耐药率 | 耐药株数 (例) | 耐药率 | 耐药株数 (例) | 耐药率 | 耐药株数 (例) | 耐药率 | 耐药株数 (例) | 耐药率 | |||
| 阿米卡星 | 0 | 0.00 | 4 | 80.00 | 1 | 20.00 | 18 | 78.26 | 53 | 100.00 | 60.543 | <0.01 |
| 阿莫西林克拉维酸 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 厄他培南 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 复方新诺明 | 0 | 0.00 | 0 | 0.00 | 0 | 0.00 | 22 | 95.65 | 50 | 94.34 | 66.333 | <0.01 |
| 替加环素 | 0 | 0.00 | 0 | 0.00 | 0 | 0.00 | 0 | 0.00 | 0 | 0.00 | / | / |
| 头孢曲松 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 头孢他啶 | 8 | 88.89 | 5 | 100.00 | 5 | 100.00 | 22 | 95.65 | 53 | 100.00 | 33.250 | <0.01 |
| 头孢西丁 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 头孢呋辛 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 头孢吡肟 | 7 | 77.78 | 3 | 60.00 | 3 | 60.00 | 23 | 100.00 | 53 | 100.00 | 33.048 | <0.01 |
| 头孢哌酮舒巴坦 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 亚胺培南 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 左氧氟沙星 | 2 | 22.22 | 3 | 60.00 | 3 | 60.00 | 22 | 95.65 | 53 | 100.00 | 51.482 | <0.01 |
| 哌拉西林他唑巴坦 | 9 | 100.00 | 5 | 100.00 | 5 | 100.00 | 23 | 100.00 | 53 | 100.00 | 47.368 | <0.01 |
| 头孢他啶阿维巴坦 | 0 | 0.00 | 0 | 0.00 | 0 | 0.00 | 0 | 0.00 | 0 | 0.00 | / | / |
| 项目 | CRKP感染组(n=95) | 非CRKP感染组(n=429) | χ2值 | P值 | |
|---|---|---|---|---|---|
| 年龄≥60岁 | 43(45.26) | 129(30.07) | 7.468 | 0.006 | |
| 男性 | 70(73.68) | 312(72.73) | 0.004 | 0.950 | |
| BMI≥24 kg/m2 | 31(32.63) | 164(38.23) | 0.817 | 0.366 | |
| 吸烟史 | 21(22.11) | 118(27.51) | 0.903 | 0.342 | |
| 饮酒史 | 21(22.11) | 63(14.69) | 2.654 | 0.103 | |
| 住院时间≥30 d | 73(76.84) | 88(20.51) | 113.313 | <0.01 | |
| 高血压史 | 34(35.79) | 112(26.11) | 3.162 | 0.075 | |
| 糖尿病史 | 14(14.74) | 72(16.78) | 0.112 | 0.738 | |
| 肿瘤 | 17(17.89) | 44(10.26) | 3.700 | 0.054 | |
| 手术 | 72(75.79) | 218(50.82) | 3.700 | 0.054 | |
| 手术时间≥60 min | 72(75.79) | 199(46.39) | 25.763 | <0.01 | |
| 手术次数≥2次 | 39(41.05) | 32(7.46) | 72.091 | <0.01 | |
| 首次手术是否术后预防用药 | 74(77.89) | 191(44.52) | 33.331 | <0.01 | |
| 抗菌药物使用时间≥30 d | 67(70.53) | 59(13.75) | 134.170 | <0.01 | |
| 联合使用抗菌药物 | 80(84.21) | 94(21.91) | 133.306 | <0.01 | |
| 使用抗菌药物种类≥3种 | 81(85.26) | 66(15.38) | 184.720 | <0.01 | |
| 入院GCS评分≤5分 | 79(83.16) | 196(45.69) | 42.298 | <0.01 | |
| 昏迷 | 81(85.26) | 299(69.70) | 8.692 | 0.003 | |
| 气管切开 | 65(68.42) | 76(17.72) | 99.111 | <0.01 | |
| 呼吸机 | 85(89.47) | 243(56.64) | 34.416 | <0.01 | |
| 留置导尿管 | 89(93.68) | 254(59.21) | 39.377 | <0.01 | |
| 中心静脉置管 | 77(81.05) | 243(56.64) | 20.164 | <0.01 | |
| 留置胃管 | 80(84.21) | 94(21.91) | 133.306 | <0.01 | |
| 二次置管 | 40(42.11) | 55(12.82) | 42.987 | <0.01 | |
| 发热≥10 d | 72(75.79) | 47(10.96) | 182.582 | <0.01 | |
| 输血 | 75(78.95) | 123(28.67) | 81.503 | <0.01 | |
| 低蛋白血症 | 86(90.53) | 190(44.29) | 64.860 | <0.01 | |
| 使用免疫抑制剂或激素 | 56(58.95) | 190(44.29) | 6.134 | 0.013 | |
Tab.2 Clinical data between the two groups (n, %)
| 项目 | CRKP感染组(n=95) | 非CRKP感染组(n=429) | χ2值 | P值 | |
|---|---|---|---|---|---|
| 年龄≥60岁 | 43(45.26) | 129(30.07) | 7.468 | 0.006 | |
| 男性 | 70(73.68) | 312(72.73) | 0.004 | 0.950 | |
| BMI≥24 kg/m2 | 31(32.63) | 164(38.23) | 0.817 | 0.366 | |
| 吸烟史 | 21(22.11) | 118(27.51) | 0.903 | 0.342 | |
| 饮酒史 | 21(22.11) | 63(14.69) | 2.654 | 0.103 | |
| 住院时间≥30 d | 73(76.84) | 88(20.51) | 113.313 | <0.01 | |
| 高血压史 | 34(35.79) | 112(26.11) | 3.162 | 0.075 | |
| 糖尿病史 | 14(14.74) | 72(16.78) | 0.112 | 0.738 | |
| 肿瘤 | 17(17.89) | 44(10.26) | 3.700 | 0.054 | |
| 手术 | 72(75.79) | 218(50.82) | 3.700 | 0.054 | |
| 手术时间≥60 min | 72(75.79) | 199(46.39) | 25.763 | <0.01 | |
| 手术次数≥2次 | 39(41.05) | 32(7.46) | 72.091 | <0.01 | |
| 首次手术是否术后预防用药 | 74(77.89) | 191(44.52) | 33.331 | <0.01 | |
| 抗菌药物使用时间≥30 d | 67(70.53) | 59(13.75) | 134.170 | <0.01 | |
| 联合使用抗菌药物 | 80(84.21) | 94(21.91) | 133.306 | <0.01 | |
| 使用抗菌药物种类≥3种 | 81(85.26) | 66(15.38) | 184.720 | <0.01 | |
| 入院GCS评分≤5分 | 79(83.16) | 196(45.69) | 42.298 | <0.01 | |
| 昏迷 | 81(85.26) | 299(69.70) | 8.692 | 0.003 | |
| 气管切开 | 65(68.42) | 76(17.72) | 99.111 | <0.01 | |
| 呼吸机 | 85(89.47) | 243(56.64) | 34.416 | <0.01 | |
| 留置导尿管 | 89(93.68) | 254(59.21) | 39.377 | <0.01 | |
| 中心静脉置管 | 77(81.05) | 243(56.64) | 20.164 | <0.01 | |
| 留置胃管 | 80(84.21) | 94(21.91) | 133.306 | <0.01 | |
| 二次置管 | 40(42.11) | 55(12.82) | 42.987 | <0.01 | |
| 发热≥10 d | 72(75.79) | 47(10.96) | 182.582 | <0.01 | |
| 输血 | 75(78.95) | 123(28.67) | 81.503 | <0.01 | |
| 低蛋白血症 | 86(90.53) | 190(44.29) | 64.860 | <0.01 | |
| 使用免疫抑制剂或激素 | 56(58.95) | 190(44.29) | 6.134 | 0.013 | |
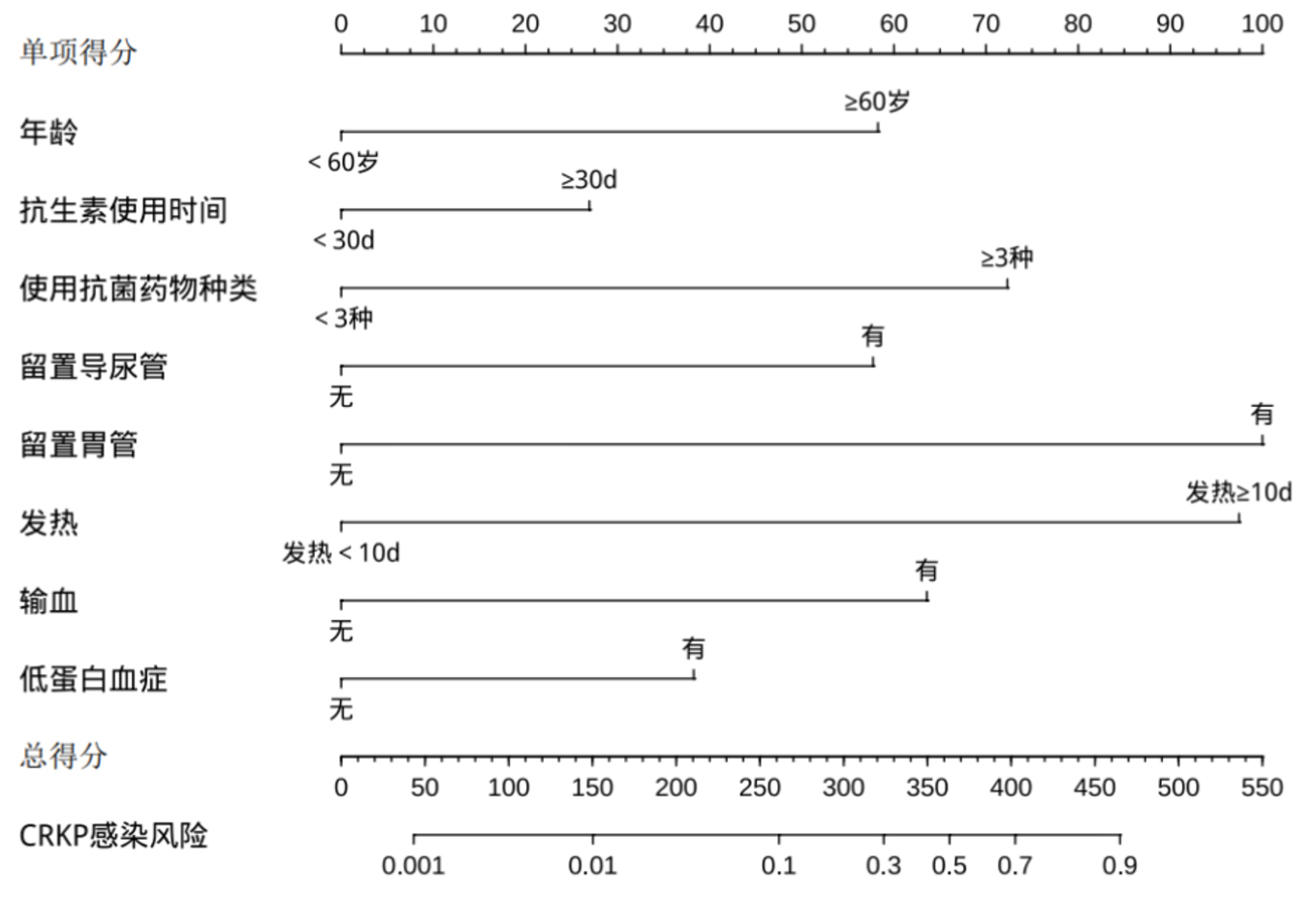
| 因素 | 回归系数 | 标准误 | Waldχ2值 | OR值 | 95%CI | P值 |
|---|---|---|---|---|---|---|
| 截距 | -6.332 | 0.993 | 40.701 | |||
| 年龄≥60岁 | 1.465 | 0.486 | 9.086 | 4.329 | 1.670~11.226 | 0.003 |
| 抗菌药物使用时间≥30 d | 1.625 | 0.687 | 5.592 | 5.081 | 1.321~19.544 | 0.018 |
| 使用抗菌药物种类≥3种 | 1.767 | 0.779 | 5.142 | 5.854 | 1.271~26.965 | 0.023 |
| 留置导尿管 | 2.456 | 0.849 | 8.368 | 11.661 | 2.208~61.590 | 0.004 |
| 留置胃管 | 3.186 | 0.842 | 14.310 | 24.179 | 4.641~125.962 | <0.01 |
| 发热≥10 d | 2.835 | 0.525 | 29.210 | 17.032 | 6.092~47.619 | <0.01 |
| 输血 | 2.184 | 0.617 | 12.529 | 8.884 | 2.651~29.779 | <0.01 |
| 低蛋白血症 | 1.334 | 0.620 | 4.631 | 3.795 | 1.126~12.788 | 0.031 |
Tab.3 Multivariate logistic regression analysis of CRKP infection in sTBI patients
| 因素 | 回归系数 | 标准误 | Waldχ2值 | OR值 | 95%CI | P值 |
|---|---|---|---|---|---|---|
| 截距 | -6.332 | 0.993 | 40.701 | |||
| 年龄≥60岁 | 1.465 | 0.486 | 9.086 | 4.329 | 1.670~11.226 | 0.003 |
| 抗菌药物使用时间≥30 d | 1.625 | 0.687 | 5.592 | 5.081 | 1.321~19.544 | 0.018 |
| 使用抗菌药物种类≥3种 | 1.767 | 0.779 | 5.142 | 5.854 | 1.271~26.965 | 0.023 |
| 留置导尿管 | 2.456 | 0.849 | 8.368 | 11.661 | 2.208~61.590 | 0.004 |
| 留置胃管 | 3.186 | 0.842 | 14.310 | 24.179 | 4.641~125.962 | <0.01 |
| 发热≥10 d | 2.835 | 0.525 | 29.210 | 17.032 | 6.092~47.619 | <0.01 |
| 输血 | 2.184 | 0.617 | 12.529 | 8.884 | 2.651~29.779 | <0.01 |
| 低蛋白血症 | 1.334 | 0.620 | 4.631 | 3.795 | 1.126~12.788 | 0.031 |
| [1] | Epstein D, Rakedzon S, Kaplan B, et al. Prevalence of significant traumatic brain injury among patients intubated in the field due to impaired level of consciousness[J]. Am J Emerg Med, 2022, 52:159-165.doi: 10.1016/j.ajem.2021.12.015. |
| [2] | Michaud J, Plu I, Parai J, et al. Ballooned neurons in semi-recent severe traumatic brain injury[J]. Acta Neuropathol Commun, 2023, 11(1):37. doi: 10.1186/s40478-023-01516-x. |
| [3] |
Goo Z, Muthusamy K. Early versus standard tracheostomy in ventilated patients in neurosurgical intensive care unit: A randomized controlled trial[J]. J Clin Neurosci, 2022, 98:162-167.doi: 10.1016/j.jocn.2022.02.011.
pmid: 35182846 |
| [4] | Thanh NQ, Cap NT, Phu VD, et al. Continuous irrigation for refractory multidrug-resistant brain abscess in two patientse[J]. Eur J Case Rep Intern Med, 2025, 12(8):005566. doi: 10.12890/2025_005566. |
| [5] | Huang H, Zhang G, Xu M, et al. The impact of tracheostomy timing on clinical outcomes and adverse events in intubated patients with infratentorial lesions: Early versus late tracheostomy[J]. Neurosurg Rev, 2023, 44(3):1513-1522.doi: 10.1007/s10143-020-01339-7. |
| [6] | Antimicrobial Resistance Collaborators. Global burden of bacterial antimicrobial resistance in 2019:A systematic analysis[J]. Lancet, 2022, 399(10325):629-655. doi: 10.1016/S0140-6736(21)02724-0. |
| [7] | Hu F, Pan Y, Li H, et al. Carbapenem-resistant Klebsiella pneumoniae capsular types, antibiotic resistance and virulence factors in China:A longitudinal,multi-centre study[J]. Nat Microbiol, 2024, 9(3):814-829. doi: 10.1038/s41564-024-01612-1. |
| [8] | Zeng M, Xia J, Zong Z, et al. Guidelines for the diagnosis,treatment,prevention and control of infections caused by carbapenem-resistant gram-negative bacilli[J]. J Microbiol Immunol Infect, 2023, 56(4):653-671.doi: 10.1016/j.jmii.2023.01.017. |
| [9] | 吕倩倩, 田金英, 李卫, 等. 血流动力学、颅内压及相关生化指标与重型颅脑损伤去骨瓣减压术后患者预后的关系及预测价值[J]. 临床医学, 2025, 45(11):1-7.doi:10.19528/j.issn.1003-3548.2025.11.001. |
| [10] | 尚红, 王毓三, 申子瑜, 等. 全国临床检验操作规程[M]. 4版. 北京: 人民卫生出版社, 2015:2335. |
| [11] | Schuetz AN, Ferrell A, Hindler JA, et al. Clinical and Laboratory Standards Institute. Performance standards for antimicrobial susceptibility testing[S]. M100-S33. Wayne,PA:CLSI, 2023. |
| [12] |
Chen L, Xia S, Lin Y, et al. The role of coagulopathy and subdural hematoma thickness at admission in predicting the prognoses of patients with severe traumatic brain injury:A multicenter retrospective cohort study from China[J]. Int J Surg, 2024, 110(9):5545-5562. doi: 10.1097/JS9.0000000000001650.
pmid: 38752515 |
| [13] | 刘爽, 王晶, 王睿, 等. ICU重症颅脑损伤术后肺部感染病原菌与血清HMGB1、ICAM-1、miR-126、miR-16表达及其意义[J]. 中华医院感染学杂志, 2024, 34(3):1992-1996. |
| [14] | 胡付品, 郭燕, 朱德妹, 等. 2019年CHINET三级医院细菌耐药监测[J]. 中国感染与化疗杂志, 2020, 20(3):233-243.doi:10.16718/j.1009-7708.2020.03.001. |
| [15] | 胡付品, 郭燕, 朱德妹, 等. 2020年CHINET中国细菌耐药监测[J]. 中国感染与化疗杂志, 2021, 21(4):377-387.doi:10.16718/j.1009-7708.2021.04.001. |
| [16] | 胡付品, 郭燕, 朱德妹, 等. 2021年CHINET中国细菌耐药监测[J]. 中国感染与化疗杂志, 2022, 22(5):521-530.doi:10.16718/j.1009-7708.2022.05.001. |
| [17] | 郭燕, 胡付品, 朱德妹, 等. 2022年CHINET三级医院细菌耐药监测[J]. 中国感染与化疗杂志, 2024, 24(3):277-286.doi:10.16718/j.1009-7708.2024.03.005. |
| [18] | 郭燕, 胡付品, 朱德妹, 等. 2023年CHINET中国细菌耐药监测[J]. 中国感染与化疗杂志, 2024, 24(6):627-637.doi:10.16718/j.1009-7708.2024.06.001. |
| [19] | Tüzemen NÜ, Önal U, Merdan O, et al. Synergistic antibacterial activity of ceftazidime-avibactam in combination with colistin, gentamicin, amikacin, and fosfomycin against carbapenem-resistant Klebsiella pneumoniae[J]. Sci Rep, 2024, 14(1):17567. doi: 10.1038/s41598-024-67347-5. |
| [20] | 郑志刚, 杜明梅, 姚宏武, 等. 2014-2023年某三甲医院血流感染耐碳青霉烯类肺炎克雷伯菌分布及耐药性变迁[J]. 中华医院感染学杂志, 2024, 34(22):3371-3375. |
| [21] | 许剑, 梁梅, 罗亚男, 等. 耐碳青霉烯类肺炎克雷伯菌肺部感染的危险因素及预后分析[J]. 中华传染病杂志, 2023, 41(11):722-726.doi:10.3760/cma.j.cn311365-20230803-00027. |
| [22] | 吴迪, 贡鑫然, 杨美涛, 等. ICU耐碳青霉烯类肺炎克雷伯菌感染危险因素的Meta分析[J]. 中华医院感染学杂志, 2022, 32(15):2241-2248. |
| [23] | Li J, Li Y, Song N, et al. Risk factors for carbapenem-resistant Klebsiella pneumoniae infection:A meta-analysis[J]. J Glob Antimicrob Resist, 2020, 21:306-313.doi: 10.1016/j.jgar.2019.09.006. |
| [24] | Krigul KL, Feeney RH, Wongkuna S, et al. A history of repeated antibiotic usage leads to microbiota-dependent mucus defects[J]. Gut Microbes, 2024, 16(1):2377570.doi: 10.1080/19490976.2024.2377570. |
| [25] | Cai S, Wang Z, Han X, et al. The correlation between intestinal colonization and infection of carbapenem-resistant Klebsiella pneumoniae: A systematic review[J]. J Glob Antimicrob Resist, 2024, 38:187-193.doi: 10.1016/j.jgar.2024.04.013. |
| [26] | Luterbach CL, Qiu H, Hanafin PO, et al. A systems-based analysis of mono- and combination therapy for carbapenem-resistant Klebsiella pneumoniae bloodstream infections[J]. Antimicrob Agents Chemother, 2022, 66(10):e0059122.doi: 10.1128/aac.00591-22. |
| [27] | Ma X, Xi W, Yang D, et al. Collateral sensitivity between tetracyclines and aminoglycosides constrains resistance evolution in carbapenem-resistant Klebsiella pneumoniae[J]. Drug Resist Updat, 2023, 68:100961.doi: 10.1016/j.drup.2023.100961. |
| [28] |
黎琪, 杨柔, 沈晓妍, 等. 重症监护病房患者多重耐药菌感染危险因素的Meta分析[J]. 医药导报, 2024, 43(10):1562-1571.
doi: 10.3870/j.issn.1004-0781.2024.10.005 |
| [29] | 贾辰, 王璐, 李海峰. ICU住院患者耐碳青霉烯类肺炎克雷伯菌感染危险因素及其BP神经网络模型的预测价值[J]. 中华医院感染学杂志, 2024, 34(12):1778-1783.doi:10.11816/cn.ni.2024-231819. |
| [30] | 杨晋如, 刘丹, 谈宜斌, 等. 重症医学科多重耐药菌感染风险因素的网状路径分析[J]. 中国感染控制杂志, 2020, 19(2):148-154. |
| [31] | Jiang H, Pu H, Huang N. Risk predict model using multi-drug resistant organism infection from Neuro-ICU patients:A retrospective cohort study[J]. Sci Rep, 2023, 13(1):15282.doi: 10.1038/s41598-023-42522-2. |
| [32] | 周淑媚, 张美萍, 方轶群, 等. 老年住院患者肺炎克雷伯菌感染危险因素及其毒力和耐药基因[J]. 中华医院感染学杂志, 2023, 33(1):35-39.doi:10.11816/cn.ni.2023-212889. |
| [33] | 唐佩娟, 欧阳鹏文, 龙晟, 等. 血液分离耐碳青霉烯类肺炎克雷伯菌耐药性及相关危险因素[J]. 中国感染控制杂志, 2024, 23(1):49-57. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||