Clinical Focus ›› 2026, Vol. 41 ›› Issue (3): 205-211.doi: 10.3969/j.issn.1004-583X.2026.03.002
Previous Articles Next Articles
Machine learning-based risk prediction model integrating multidimensional risk factors for rehospitalization in acute decompensated heart failure
Zhu Menglia( ), Li Minb, Xue Shashac, Wei Miaomiaoc, Fu Huijuanc
), Li Minb, Xue Shashac, Wei Miaomiaoc, Fu Huijuanc
- a. Quality Control Office; b.General Office; c.Department of Cardiovascular Medicine, Yellow River Sanmenxia Hospital, Sanmenxia 472000, China
-
Received:2026-02-26Online:2026-03-20Published:2026-03-27
CLC Number:
Cite this article
Zhu Mengli, Li Min, Xue Shasha, Wei Miaomiao, Fu Huijuan. Machine learning-based risk prediction model integrating multidimensional risk factors for rehospitalization in acute decompensated heart failure[J]. Clinical Focus, 2026, 41(3): 205-211.
share this article
Add to citation manager EndNote|Ris|BibTeX
URL: https://www.lchc.cn/EN/10.3969/j.issn.1004-583X.2026.03.002
| 因素 | 再住院组(n=72) | 对照组(n=152) | χ2值 | P值 | |
|---|---|---|---|---|---|
| 年龄[例(%)] | |||||
| ≥60岁 <60岁 | 48(66.67) 24(33.33) | 95(62.50) 57(37.50) | 0.367 | 0.544 | |
| 性别[例(%)] | |||||
| 男 女 | 34(47.22) 38(52.78) | 65(42.76) 87(57.24) | 0.394 | 0.530 | |
| 体质量指数[例(%)] | |||||
| <18.5 kg/m2 | 15(20.84) | 32(21.05) | |||
| 18.5~23.9 kg/m2 | 43(59.72) | 80(52.63) | 1.405 | 0.495 | |
| >23.9 kg/m2 | 14(19.44) | 40(26.32) | |||
| 文化程度[例(%)] | |||||
| 初中及以下 高中及以上 | 32(44.44) 40(55.56) | 60(39.47) 92(60.53) | 0.499 | 0.480 | |
| 居住情况[例(%)] | |||||
| 独居 与配偶/子女同住 | 42(58.33) 30(41.67) | 42(27.63) 110(72.37) | 19.649 | <0.001 | |
| 病程[例(%)] | |||||
| <1年 | 20(27.78) | 68(44.74) | |||
| 1~5年 | 18(25.00) | 50(32.89) | 14.521 | 0.001 | |
| >5年 | 34(47.22) | 34(22.37) | |||
| 出院时NYHA心功能分级[例(%)] | |||||
| Ⅱ、Ⅲ级 Ⅳ级 | 32(44.44) 40(55.56) | 92(60.53) 60(39.47) | 5.113 | 0.024 | |
| 规律复诊[例(%)] | |||||
| 是 否 | 52(72.22) 20(27.78) | 130(85.53) 22(14.47) | 5.676 | 0.017 | |
| 坚持低钠饮食[例(%)] | |||||
| 是 否 | 50(69.44) 22(30.56) | 132(86.84) 20(13.16) | 9.707 | 0.002 | |
| 坚持限制饮水[例(%)] | |||||
| 是 否 | 33(45.83) 39(54.17) | 100(65.79) 52(34.21) | 8.066 | 0.005 | |
| 服药依从性[例(%)] | |||||
| 好 差 | 52(72.22) 20(83.55) | 127(83.55) 25(16.45) | 3.907 | 0.048 | |
| 自理能力[例(%)] | |||||
| 有 无 | 57(79.17) 15(20.83) | 140(92.11) 12(7.89) | 7.716 | 0.005 | |
| 焦虑[例(%)] | |||||
| 是 否 | 20(27.78) 52(72.22) | 23(15.13) 129(84.87) | 5.037 | 0.025 | |
| 抑郁[例(%)] | |||||
| 是 否 | 17(23.61) 55(76.39) | 20(13.16) 132(86.84) | 3.872 | 0.049 | |
| 适当运动[例(%)] | |||||
| 是 否 | 50(69.44) 22(30.56) | 132(86.84) 20(13.16) | 9.707 | 0.002 | |
| 高血压[例(%)] | |||||
| 是 否 | 40(55.56) 32(44.44) | 69(45.39) 83(54.61) | 2.019 | 0.155 | |
| 糖尿病[例(%)] | |||||
| 是 否 | 22(30.56) 50(69.44) | 43(28.29) 109(71.71) | 0.122 | 0.727 | |
| 高血脂[例(%)] | |||||
| 是 否 | 42(58.33) 30(41.67) | 67(44.08) 85(55.92) | 3.974 | 0.046 | |
| 吸烟史[例(%)] | |||||
| 是 否 | 25(34.72) 47(65.28) | 67(44.08) 85(55.92) | 1.767 | 0.184 | |
| 饮酒史[例(%)] | |||||
| 是 否 | 30(41.67) 42(58.33) | 49(32.24) 103(67.76) | 1.903 | 0.168 | |
Tab.1 Univariate analysis of factors influencing rehospitalization in ADHF patients
| 因素 | 再住院组(n=72) | 对照组(n=152) | χ2值 | P值 | |
|---|---|---|---|---|---|
| 年龄[例(%)] | |||||
| ≥60岁 <60岁 | 48(66.67) 24(33.33) | 95(62.50) 57(37.50) | 0.367 | 0.544 | |
| 性别[例(%)] | |||||
| 男 女 | 34(47.22) 38(52.78) | 65(42.76) 87(57.24) | 0.394 | 0.530 | |
| 体质量指数[例(%)] | |||||
| <18.5 kg/m2 | 15(20.84) | 32(21.05) | |||
| 18.5~23.9 kg/m2 | 43(59.72) | 80(52.63) | 1.405 | 0.495 | |
| >23.9 kg/m2 | 14(19.44) | 40(26.32) | |||
| 文化程度[例(%)] | |||||
| 初中及以下 高中及以上 | 32(44.44) 40(55.56) | 60(39.47) 92(60.53) | 0.499 | 0.480 | |
| 居住情况[例(%)] | |||||
| 独居 与配偶/子女同住 | 42(58.33) 30(41.67) | 42(27.63) 110(72.37) | 19.649 | <0.001 | |
| 病程[例(%)] | |||||
| <1年 | 20(27.78) | 68(44.74) | |||
| 1~5年 | 18(25.00) | 50(32.89) | 14.521 | 0.001 | |
| >5年 | 34(47.22) | 34(22.37) | |||
| 出院时NYHA心功能分级[例(%)] | |||||
| Ⅱ、Ⅲ级 Ⅳ级 | 32(44.44) 40(55.56) | 92(60.53) 60(39.47) | 5.113 | 0.024 | |
| 规律复诊[例(%)] | |||||
| 是 否 | 52(72.22) 20(27.78) | 130(85.53) 22(14.47) | 5.676 | 0.017 | |
| 坚持低钠饮食[例(%)] | |||||
| 是 否 | 50(69.44) 22(30.56) | 132(86.84) 20(13.16) | 9.707 | 0.002 | |
| 坚持限制饮水[例(%)] | |||||
| 是 否 | 33(45.83) 39(54.17) | 100(65.79) 52(34.21) | 8.066 | 0.005 | |
| 服药依从性[例(%)] | |||||
| 好 差 | 52(72.22) 20(83.55) | 127(83.55) 25(16.45) | 3.907 | 0.048 | |
| 自理能力[例(%)] | |||||
| 有 无 | 57(79.17) 15(20.83) | 140(92.11) 12(7.89) | 7.716 | 0.005 | |
| 焦虑[例(%)] | |||||
| 是 否 | 20(27.78) 52(72.22) | 23(15.13) 129(84.87) | 5.037 | 0.025 | |
| 抑郁[例(%)] | |||||
| 是 否 | 17(23.61) 55(76.39) | 20(13.16) 132(86.84) | 3.872 | 0.049 | |
| 适当运动[例(%)] | |||||
| 是 否 | 50(69.44) 22(30.56) | 132(86.84) 20(13.16) | 9.707 | 0.002 | |
| 高血压[例(%)] | |||||
| 是 否 | 40(55.56) 32(44.44) | 69(45.39) 83(54.61) | 2.019 | 0.155 | |
| 糖尿病[例(%)] | |||||
| 是 否 | 22(30.56) 50(69.44) | 43(28.29) 109(71.71) | 0.122 | 0.727 | |
| 高血脂[例(%)] | |||||
| 是 否 | 42(58.33) 30(41.67) | 67(44.08) 85(55.92) | 3.974 | 0.046 | |
| 吸烟史[例(%)] | |||||
| 是 否 | 25(34.72) 47(65.28) | 67(44.08) 85(55.92) | 1.767 | 0.184 | |
| 饮酒史[例(%)] | |||||
| 是 否 | 30(41.67) 42(58.33) | 49(32.24) 103(67.76) | 1.903 | 0.168 | |
| 变量 | 赋值 |
|---|---|
| 因变量(Y) | |
| ADHF患者是否发生再住院 | 是=1,否=0 |
| 自变量(X) | |
| 出院时NYHA心功能分级 | Ⅱ、Ⅲ级=0,Ⅳ级=1 |
| 规律复诊 | 是=1,否=0 |
| 坚持低钠饮食 | 是=1,否=0 |
| 服药依从性 | 好=0,差=1 |
| 焦虑 | 是=1,否=0 |
| 抑郁 | 是=1,否=0 |
| 适当运动 | 是=1,否=0 |
| 高血脂 | 是=1,否=0 |
Tab.2 Coding/assignment table for multivariate logistic regression
| 变量 | 赋值 |
|---|---|
| 因变量(Y) | |
| ADHF患者是否发生再住院 | 是=1,否=0 |
| 自变量(X) | |
| 出院时NYHA心功能分级 | Ⅱ、Ⅲ级=0,Ⅳ级=1 |
| 规律复诊 | 是=1,否=0 |
| 坚持低钠饮食 | 是=1,否=0 |
| 服药依从性 | 好=0,差=1 |
| 焦虑 | 是=1,否=0 |
| 抑郁 | 是=1,否=0 |
| 适当运动 | 是=1,否=0 |
| 高血脂 | 是=1,否=0 |
| 因素 | β | SE | Waldχ2值 | P值 | OR值 | 95%可信区间 |
|---|---|---|---|---|---|---|
| 出院时NYHA心功能分级 | 0.658 | 0.246 | 7.155 | <0.001 | 1.431 | 1.204~3.268 |
| 规律复诊 | -0.679 | 0.278 | 5.966 | <0.001 | 0.507 | 0.289~0.930 |
| 坚持低钠饮食 | -0.632 | 0.258 | 6.001 | <0.001 | 0.532 | 0.276~0.858 |
| 服药依从性 | 0.703 | 0.312 | 5.077 | <0.001 | 1.520 | 1.208~4.750 |
| 焦虑 | 0.396 | 0.128 | 9.576 | 0.002 | 1.486 | 1.126~4.058 |
| 抑郁 | 0.599 | 0.263 | 5.187 | <0.001 | 1.520 | 1.152~4.167 |
| 适当运动 | -0.639 | 0.279 | 5.246 | <0.001 | 0.528 | 0.255~0.889 |
| 高血脂 | 0.681 | 0.257 | 7.021 | <0.001 | 1.976 | 1.227~2.852 |
Tab.3 Multivariate logistic regression analysis of factors associated with rehospitalization in ADHF patients
| 因素 | β | SE | Waldχ2值 | P值 | OR值 | 95%可信区间 |
|---|---|---|---|---|---|---|
| 出院时NYHA心功能分级 | 0.658 | 0.246 | 7.155 | <0.001 | 1.431 | 1.204~3.268 |
| 规律复诊 | -0.679 | 0.278 | 5.966 | <0.001 | 0.507 | 0.289~0.930 |
| 坚持低钠饮食 | -0.632 | 0.258 | 6.001 | <0.001 | 0.532 | 0.276~0.858 |
| 服药依从性 | 0.703 | 0.312 | 5.077 | <0.001 | 1.520 | 1.208~4.750 |
| 焦虑 | 0.396 | 0.128 | 9.576 | 0.002 | 1.486 | 1.126~4.058 |
| 抑郁 | 0.599 | 0.263 | 5.187 | <0.001 | 1.520 | 1.152~4.167 |
| 适当运动 | -0.639 | 0.279 | 5.246 | <0.001 | 0.528 | 0.255~0.889 |
| 高血脂 | 0.681 | 0.257 | 7.021 | <0.001 | 1.976 | 1.227~2.852 |
| 模型类别 | 敏感度(%) | 特异度(%) | 准确率(%) | AUC |
|---|---|---|---|---|
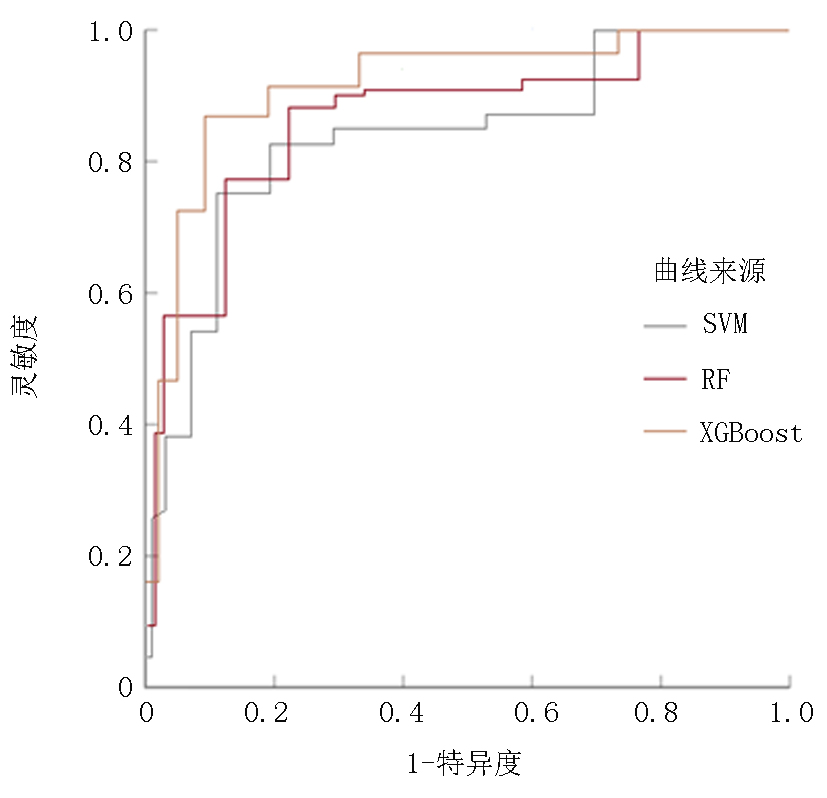
| SVM | 83.33(60/72) | 65.79(100/152) | 71.43(160/224) | 0.823 |
| RF | 69.44(50/72) | 78.95(120/152) | 75.89(170/224) | 0.869 |
| XGBoost | 88.89(64/72) | 82.24(125/152) | 84.38(189/224) | 0.916 |
Tab.4 ROC parameters for SVM, RF, and XGBoost models predicting rehospitalization in ADHF patients
| 模型类别 | 敏感度(%) | 特异度(%) | 准确率(%) | AUC |
|---|---|---|---|---|
| SVM | 83.33(60/72) | 65.79(100/152) | 71.43(160/224) | 0.823 |
| RF | 69.44(50/72) | 78.95(120/152) | 75.89(170/224) | 0.869 |
| XGBoost | 88.89(64/72) | 82.24(125/152) | 84.38(189/224) | 0.916 |
| [1] | Niforatos JD, Ehmann MR, Balhara KS, et al. Management of atrial flutter and atrial fibrillation with rapid ventricular response in patients with acute decompensated heart failure: A systematic review[J]. Acad Emerg Med, 2023, 30(2):124-132. doi: 10.1111/acem.14618. |
| [2] |
Frea S, Gravinese C, Boretto P, et al. Comprehensive non-invasive haemodynamic assessment in acute decompensated heart failure-related cardiogenic shock: A step towards echodynamics[J]. Eur Heart J Acute Cardiovasc Care, 2024, 13(9):646-655.doi: 10.1093/ehjacc/zuae087.
pmid: 39012797 |
| [3] | Schulze PC, Bogoviku J, Westphal J, et al. Effects of early empagliflozin initiation on diuresis and kidney function in patients with acute decompensated heart failure (EMPAG-HF)[J]. Circulation, 2022, 146(4):289-298. doi: 10.1161/CIRCULATIONAHA.122.059038. |
| [4] | Triska J, Tamargo J, Bozkurt B, et al. An updated review on the role of non-dihydropyridine calcium channel blockers and beta-blockers in atrial fibrillation and acute decompensated heart failure: Evidence and gaps[J]. Cardiovasc Drugs Ther, 2023, 37(6):1205-1223. doi: 10.1007/s10557-022-07334-y. |
| [5] |
Zhao Z, Wang W, Jin J, et al. Diagnosis for readmission of senile patients hospitalized with acute decompensated heart failure in different departments: A retrospective cross-sectional study[J]. J Thorac Dis, 2022, 14(5):1556-1562.doi: 10.21037/jtd-22-433.
pmid: 35693607 |
| [6] | Vural A, Aydın E. The predictive value of eosinophil indices for major cardiovascular events in patients with acute decompensated HFrEF[J]. Medicina (Kaunas), 2022, 58(10):1455. doi: 10.3390/medicina58101455. |
| [7] | Lin J, Gu C, Sun Z, et al. Machine learning-based model for predicting the occurrence and mortality of nonpulmonary sepsis-associated ARDS[J]. Sci Rep, 2024, 14(1):28240.doi: 10.1038/s41598-024-79899-7. |
| [8] |
Hounye AH, Xiong L, Hou M. Integrated explainable machine learning and multi-omics analysis for survival prediction in cancer with immunotherapy response[J]. Apoptosis, 2025, 30(1-2):364-388.doi: 10.1007/s10495-024-02050-4.
pmid: 39633110 |
| [9] | Faragli A, Tano GD, Carlini C, et al. In-hospital heart rate reduction with beta blockers and ivabradine early after recovery in patients with acute decompensated heart failure reduces short-term mortality and rehospitalization[J]. Front Cardiovasc Med, 2021, 8(13):665202. doi: 10.3389/fcvm.2021.665202. |
| [10] | Okoye C, Mazzarone T, Niccolai F, et al. Predicting mortality and re-hospitalization for heart failure: A machine-learning and cluster analysis on frailty and comorbidity[J]. Aging Clin Exp Res, 2023, 35(12):2919-2928. doi: 10.1007/s40520-023-02566-w. |
| [11] | Hafkamp FJ, Tio RA, Otterspoor LC, et al. Optimal effectiveness of heart failure management-an umbrella review of meta-analyses examining the effectiveness of interventions to reduce (re)hospitalizations in heart failure[J]. Heart Fail Rev, 2022, 27(5):1683-1748.doi: 10.1007/s10741-021-10212-8. |
| [12] | Hida Y, Imamura T, Kinugawa K. Optimal timing of vericiguat therapy in patients with heart failure with reduced/mildly reduced ejection fraction for improving mortality and heart failure re-hospitalization rate[J]. J Clin Med, 2025, 14(16):5856. doi: 10.3390/jcm14165856. |
| [13] | 李佳欢, 王璐, 曲静, 等. 慢性心力衰竭患者再入院调查及影响因素分析[J]. 华南预防医学, 2024, 50(4):323-328.doi:10.12183/j.scjpm.2024.0323. |
| [14] | 陈丽娜, 付丽, 卢薇薇. 急性失代偿性心力衰竭患者血清钠离子和尿酸水平及患者的心理调适对短期预后的影响[J]. 心脑血管病防治, 2023, 23(10):52-54.doi:10.3969/j.issn.1009-816x.2023.10.012. |
| [15] | Zaghi A, Holm H, Korduner J, et al. Physical inactivity is associated with post-discharge mortality and re-hospitalization risk among swedish heart failure patients-the harvest-malmö study[J]. Front Cardiovasc Med, 2022, 9(25):843029.doi: 10.3389/fcvm.2022.843029. |
| [16] | Lucki M, Mitkowski P, Lucka E, et al. Risk factors for prolonged hospitalization in acute decompensated heart failure from the HEROES study[J]. Sci Rep, 2025, 15(1):29133.doi: 10.1038/s41598-025-14100-1. |
| [17] | 杨红梅, 李海珍, 刘娟, 等. 慢性心力衰竭患者1年内再入院情况及影响因素分析[J]. 华南预防医学, 2023, 49(6):676-680.doi:10.12183/j.scjpm.2023.0676. |
| [18] | Kumar A, Kapoor A, Harikrishnan S, et al. Prediction of incident heart failure and/or re-hospitalization using different risk predictor models in Indian patients[J]. Indian Heart J, 2025:S0019- 4832(25)00173-7. doi: 10.1016/j.ihj.2025.09.005. |
| [19] | Hu Y, Ma F, Hu M, et al. Development and validation of a machine learning model to predict the risk of readmission within one year in HFpEF patients: Short title: Prediction of HFpEF readmission[J]. Int J Med Inform, 2025, 194:105703.doi: 10.1016/j.ijmedinf.2024.105703. |
| [20] | Jiang Y, Wang HW, et al. Predicting carbapenem-resistant Pseudomonas aeruginosa infection risk using XGBoost model and explainability[J]. Sci Rep, 2025, 15(1):19737.doi: 10.1038/s41598-025-04028-x. |
| [21] | Yuan ZN, Xue YJ, Wang HJ, et al. A predictive model for hospital death in cancer patients with acute pulmonary embolism using XGBoost machine learning and SHAP interpretation[J]. Sci Rep, 2025, 15(1):18268.doi: 10.1038/s41598-025-02072-1. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||