Clinical Focus ›› 2026, Vol. 41 ›› Issue (3): 228-234.doi: 10.3969/j.issn.1004-583X.2026.03.006
Previous Articles Next Articles
Multi-center management of arteriovenous fistulas for hemodialysis with a single venous outflow tract in the antecubital perforating vein
Cheng Huidong1, Lou Wenyuan1, Liu Tongqiang2, Li Jing1, Mao Wenbin2, Mou Hongbin3, He Jianqiang1( )
)
- 1. Department of Nephrology, Affiliated Hospital of Jiangsu University, Zhenjiang 212000, China
2. Department of Nephrology, Changzhou Second People's Hospital, Changzhou 213000, China
3. Department of Nephrology, Northern Jiangsu People's Hospital, Yangzhou 225000, China
-
Received:2026-01-07Online:2026-03-20Published:2026-03-27
CLC Number:
Cite this article
Cheng Huidong, Lou Wenyuan, Liu Tongqiang, Li Jing, Mao Wenbin, Mou Hongbin, He Jianqiang. Multi-center management of arteriovenous fistulas for hemodialysis with a single venous outflow tract in the antecubital perforating vein[J]. Clinical Focus, 2026, 41(3): 228-234.
share this article
Add to citation manager EndNote|Ris|BibTeX
URL: https://www.lchc.cn/EN/10.3969/j.issn.1004-583X.2026.03.006
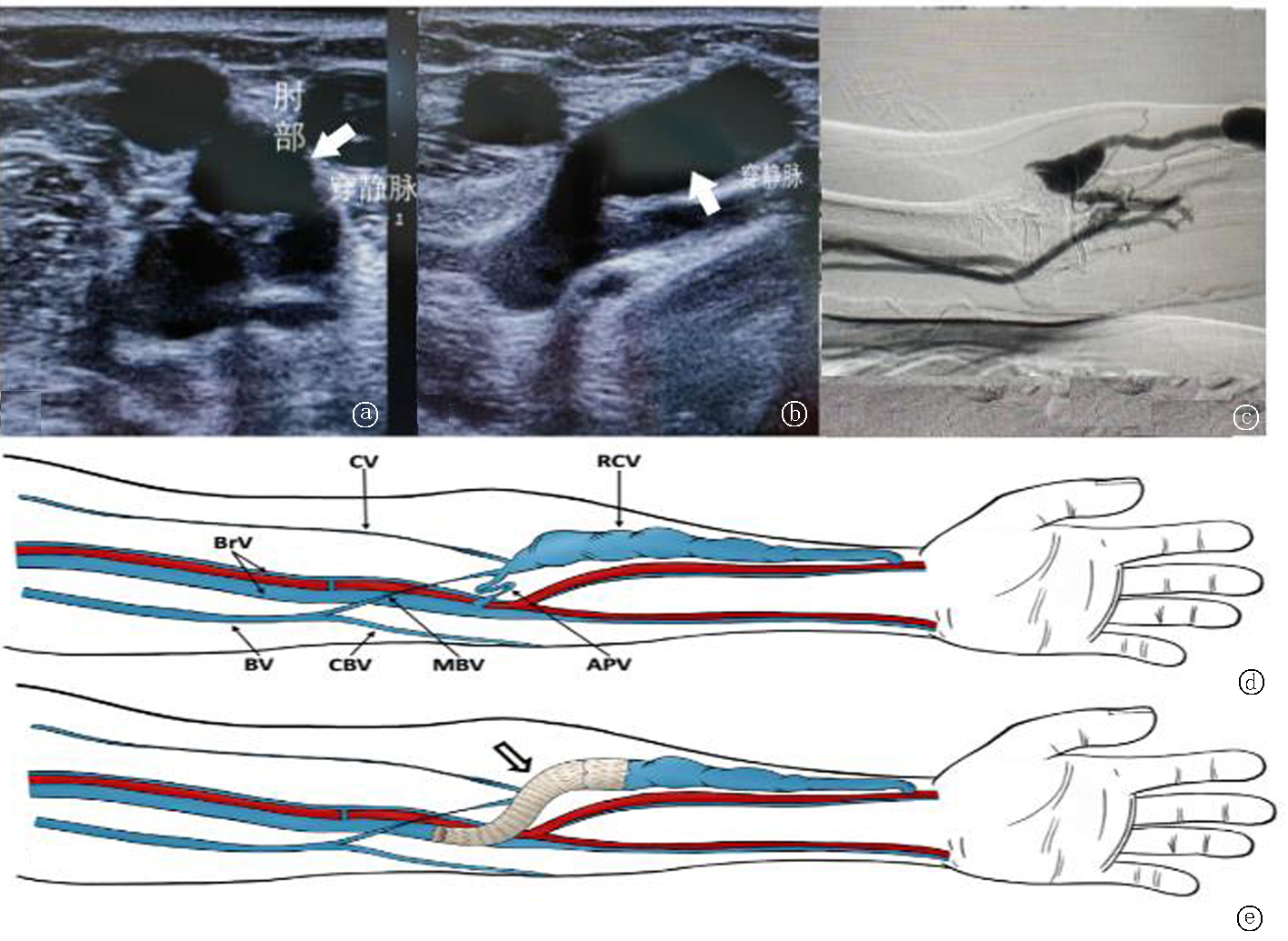
Fig.1 Ultrasound scan, contrast imaging and schematic diagram of dysfunctional AVF with a single outflow tract in APV a. Transverse section, b. Longitudinal section: Ultrasound shows stenosis and occlusion of MBV and CV, while APV is open and knotted (white arrow); c. Contrast imaging: The MBV, CV branches and vital veins in the middle section of the forearm were not visualized. The contrast agent flowed into the deep veins through the APV, and the blood vessels at the elbow were in a reverse "Z" shape. D. e. Schematic diagram: Radial vein that only drains to the brachial vein through APV, with CV and MBV of the upper arm occluded; A covered stent (indicated by the white arrow) was implanted at the APV to open up blood flow.
| 项目 | 数值 |
|---|---|
| 年龄(岁) | 64.55±11.58 |
| 男[例(%)] | 13(48.15) |
| 透析龄(月) | 52.00(30.00, 146.00) |
| 原发病[例(%)] | |
| 糖尿病 | 8(29.63) |
| 高血压病 | 6(22.22) |
| 原发性肾小球疾病 | 3(11.11) |
| 自身免疫相关肾脏病 | 2(7.41) |
| 病因不明 | 8(29.63) |
| AVF建立时间(月) | 50.00(17.00,124.00) |
| 确诊时化验资料 | |
| 血红蛋白(g/L) | 99.22±12.07 |
| 白蛋白(g/L) | 37.69±1.29 |
| 血肌酐(μmol/L) | 906.75±114.73 |
| 血尿素氮(mmol/L) | 24.29±3.94 |
| 胆固醇(mmol/L) | 3.70±1.00 |
| 甘油三酯(mmol/L) | 1.40(1.16, 1.87) |
| 钾(mmol/L) | 4.23(3.94,4.98) |
| 磷(mmol/L) | 1.74(1.38,2.00) |
| 钙(mmol/L) | 2.03(2.00, 2.09) |
| 甲状旁腺激素(pg/ml) | 362.89±124.28 |
| D-二聚体(mg/L) | 0.38(0.14, 0.64) |
| 临床表现[例(%)] | |
| 震颤减弱 | 5(18.52) |
| 震颤消失 | 9(33.33) |
| 流量下降 | 7(25.93) |
| 静脉压高 | 2(7.41) |
| 疼痛 | 3(11.11) |
| 其他 | 1(3.70) |
| 血栓形成[例(%)] | 13(48.15) |
Tab.1 General information of patients(n=27)
| 项目 | 数值 |
|---|---|
| 年龄(岁) | 64.55±11.58 |
| 男[例(%)] | 13(48.15) |
| 透析龄(月) | 52.00(30.00, 146.00) |
| 原发病[例(%)] | |
| 糖尿病 | 8(29.63) |
| 高血压病 | 6(22.22) |
| 原发性肾小球疾病 | 3(11.11) |
| 自身免疫相关肾脏病 | 2(7.41) |
| 病因不明 | 8(29.63) |
| AVF建立时间(月) | 50.00(17.00,124.00) |
| 确诊时化验资料 | |
| 血红蛋白(g/L) | 99.22±12.07 |
| 白蛋白(g/L) | 37.69±1.29 |
| 血肌酐(μmol/L) | 906.75±114.73 |
| 血尿素氮(mmol/L) | 24.29±3.94 |
| 胆固醇(mmol/L) | 3.70±1.00 |
| 甘油三酯(mmol/L) | 1.40(1.16, 1.87) |
| 钾(mmol/L) | 4.23(3.94,4.98) |
| 磷(mmol/L) | 1.74(1.38,2.00) |
| 钙(mmol/L) | 2.03(2.00, 2.09) |
| 甲状旁腺激素(pg/ml) | 362.89±124.28 |
| D-二聚体(mg/L) | 0.38(0.14, 0.64) |
| 临床表现[例(%)] | |
| 震颤减弱 | 5(18.52) |
| 震颤消失 | 9(33.33) |
| 流量下降 | 7(25.93) |
| 静脉压高 | 2(7.41) |
| 疼痛 | 3(11.11) |
| 其他 | 1(3.70) |
| 血栓形成[例(%)] | 13(48.15) |
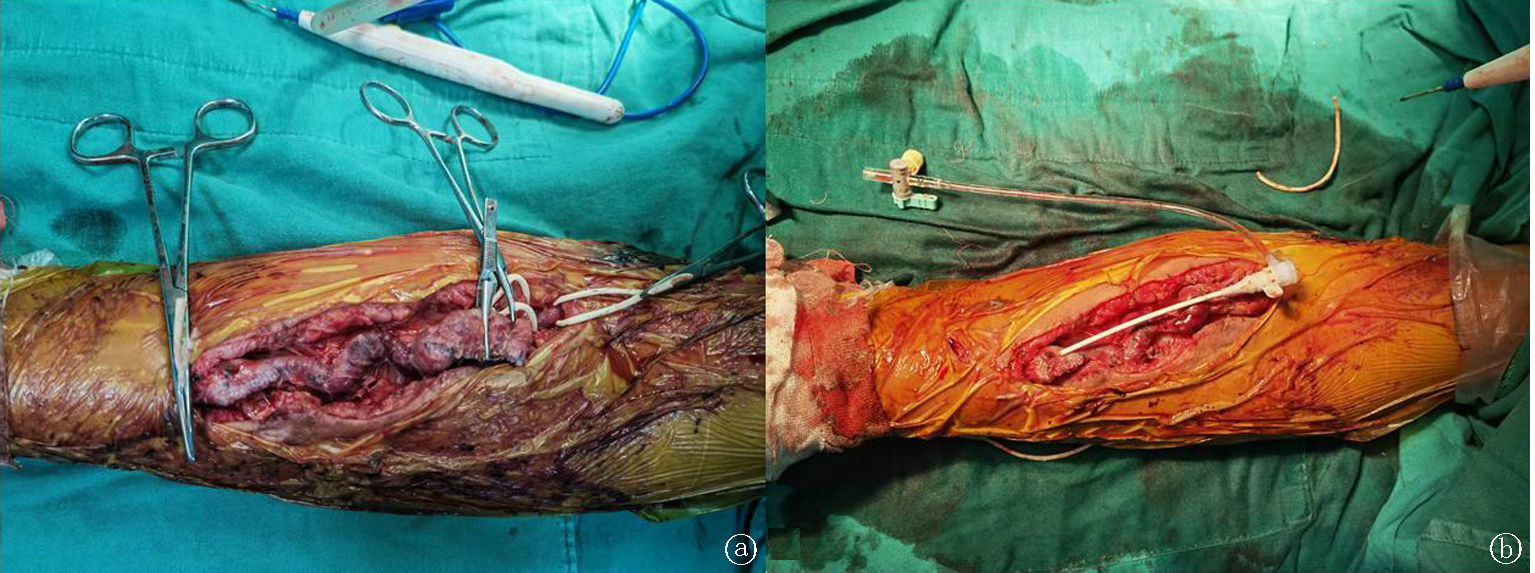
Fig.3 Surgical diagram of one case of APV outflow tract obstruction accompanied by an aneurysm A patient with post-anastomotic aneurysm and whole-course venous thrombosis was treated by a complicated surgery. a: After thrombectomy, aneurysm resection, AVF repair, and APV-BRV anastomosis; b: PTA dilation stenosis section CV; AVF was successfully activated 4 weeks after the operation.
| 项目 | 总手术次数(n=29) | 江苏大学附属医院(n=20) | 常州市第二人民医院(n=6) | 苏北人民医院(n=3) |
|---|---|---|---|---|
| AVG | 12 | 7 | 2 | 3 |
| PTA | 7 | 6 | 1 | 0 |
| 血管转位 | 8 | 7 | 1 | 0 |
| 自体血管间置 | 1 | 0 | 1 | 0 |
| BV-尺动脉AVF | 1 | 0 | 1 | 0 |
Tab.2 Date summary of surgeries in each center(n)
| 项目 | 总手术次数(n=29) | 江苏大学附属医院(n=20) | 常州市第二人民医院(n=6) | 苏北人民医院(n=3) |
|---|---|---|---|---|
| AVG | 12 | 7 | 2 | 3 |
| PTA | 7 | 6 | 1 | 0 |
| 血管转位 | 8 | 7 | 1 | 0 |
| 自体血管间置 | 1 | 0 | 1 | 0 |
| BV-尺动脉AVF | 1 | 0 | 1 | 0 |
| 组别 | 手术 次数 | 技术成功率 [例(%)] | 并发症 [例(%)] | 随访时间 (月) | 初级通畅率[例(%)] | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 6月 | 12月 | 18月 | 24月 | ||||||||||
| 总数 | 29 | 26(89.66) | 3(10.34) | 21.00(11.75,27.50) | 22(88.50) | 13(69.80) | 5(41.90) | 2(41.90) | |||||
| AVG | 12 | 12(100.00) | 2(16.70) | 22.50(13.75,63.75) | 10(83.30) | 7(64.80) | 2(21.60) | / | |||||
| 血管转位 | 8 | 8(100.00) | 0 | 19.50(13.00,25.25) | 8(100.00) | 5(75.00) | 2(75.00) | 1(75.00) | |||||
| PTA | 7 | 4(57.14) | 1(14.29) | 8.50(5.00,10.50) | 3(100.00) | / | / | / | |||||
| 其他 | 2 | 2(100.00) | 0 | 24.50(23.00,24.50) | 1(50.00) | 1(50.00) | 1(50.00) | 1(50.00) | |||||
| χ2/Z值 | 10.516 | 1.788 | 6.834 | 5.349 | 0.673 | 1.122 | 1.406 | ||||||
| P值 | 0.017 | 0.672 | 0.107 | 0.217 | 0.652 | 0.408 | 0.378 | ||||||
| 组别 | 次级通畅率[例(%)] | 总通畅率 [例(%)] | 再手术概率 (次/人) | ||||||||||
| 6月 | 12月 | 18月 | 24月 | ||||||||||
| 总数 | 25(100.00) | 19(100.00) | 15(100.00) | 9(100.00) | 22(84.61) | 1.12 | |||||||
| AVG | 12(100.00) | 10(100.00) | 9(100.00) | 5(100.00) | 8(66.70) | 1.67 | |||||||
| 血管转位 | 8(100.00) | 7(100.00) | 4(100.00) | 2(100.00) | 8(100.00) | 0.75 | |||||||
| PTA | 3(100.00) | / | / | / | 3(75.00) | 0.50 | |||||||
| 其他 | 2(100.00) | 2(100.00) | 2(100.00) | 2(100.00) | 2(100.00) | 0.50 | |||||||
| χ2/Z值 | / | / | / | / | 1.651 | 9.365 | |||||||
| P值 | / | / | / | / | 0.362 | 0.027 | |||||||
Tab.3 Surgical outcomes and follow-up for the patients
| 组别 | 手术 次数 | 技术成功率 [例(%)] | 并发症 [例(%)] | 随访时间 (月) | 初级通畅率[例(%)] | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 6月 | 12月 | 18月 | 24月 | ||||||||||
| 总数 | 29 | 26(89.66) | 3(10.34) | 21.00(11.75,27.50) | 22(88.50) | 13(69.80) | 5(41.90) | 2(41.90) | |||||
| AVG | 12 | 12(100.00) | 2(16.70) | 22.50(13.75,63.75) | 10(83.30) | 7(64.80) | 2(21.60) | / | |||||
| 血管转位 | 8 | 8(100.00) | 0 | 19.50(13.00,25.25) | 8(100.00) | 5(75.00) | 2(75.00) | 1(75.00) | |||||
| PTA | 7 | 4(57.14) | 1(14.29) | 8.50(5.00,10.50) | 3(100.00) | / | / | / | |||||
| 其他 | 2 | 2(100.00) | 0 | 24.50(23.00,24.50) | 1(50.00) | 1(50.00) | 1(50.00) | 1(50.00) | |||||
| χ2/Z值 | 10.516 | 1.788 | 6.834 | 5.349 | 0.673 | 1.122 | 1.406 | ||||||
| P值 | 0.017 | 0.672 | 0.107 | 0.217 | 0.652 | 0.408 | 0.378 | ||||||
| 组别 | 次级通畅率[例(%)] | 总通畅率 [例(%)] | 再手术概率 (次/人) | ||||||||||
| 6月 | 12月 | 18月 | 24月 | ||||||||||
| 总数 | 25(100.00) | 19(100.00) | 15(100.00) | 9(100.00) | 22(84.61) | 1.12 | |||||||
| AVG | 12(100.00) | 10(100.00) | 9(100.00) | 5(100.00) | 8(66.70) | 1.67 | |||||||
| 血管转位 | 8(100.00) | 7(100.00) | 4(100.00) | 2(100.00) | 8(100.00) | 0.75 | |||||||
| PTA | 3(100.00) | / | / | / | 3(75.00) | 0.50 | |||||||
| 其他 | 2(100.00) | 2(100.00) | 2(100.00) | 2(100.00) | 2(100.00) | 0.50 | |||||||
| χ2/Z值 | / | / | / | / | 1.651 | 9.365 | |||||||
| P值 | / | / | / | / | 0.362 | 0.027 | |||||||
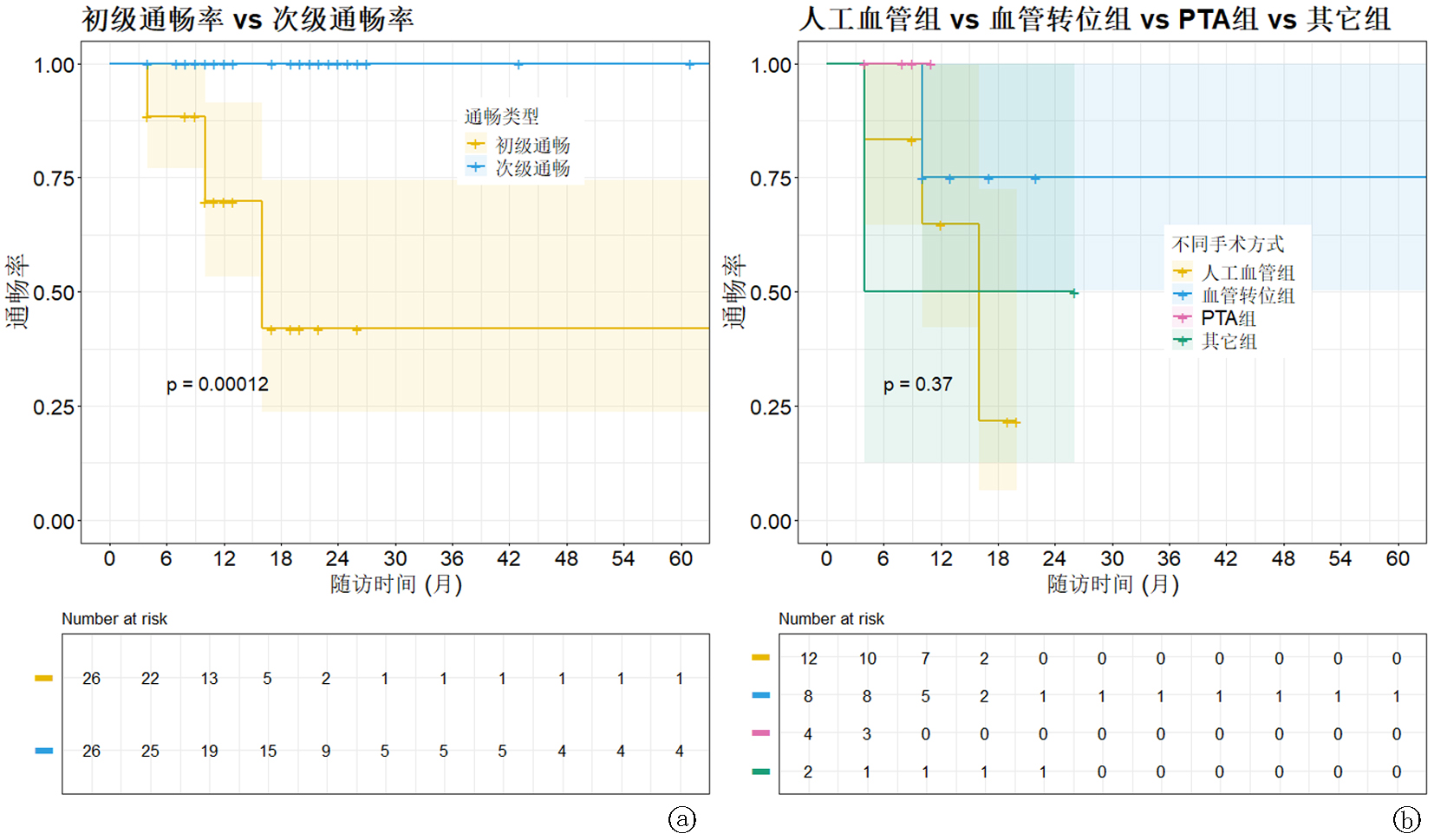
Fig.4 Patency rate (K-M curve) a. Comparison of the initial and secondary patency rates for all patients; b. Comparison of the primary patency rates among the four groups.
| [1] | Schmidli J, Widmer MK, Basile C, et al. Editor's choice - vascular access: 2018 Clinical practice guidelines of the European Society for Vascular Surgery (ESVS)[J]. Eur J Vasc Endovasc Surg, 2018, 55(6): 757-818. doi:10.1016/j.ejvs.2018.02.001. |
| [2] |
Pirozzi N, Garcia-Medina J, Hanoy M. Stenosis complicating vascular access for hemodialysis: Indications for treatment[J]. J Vasc Access, 2014, 15(2): 76-82. doi:10.5301/jva.5000194.
pmid: 24190072 |
| [3] |
Pirozzi N, De Alexandris L, Fazzari L, et al. Cubital vein transposition for a distal radiocephalic fistula complicated by outflow obstruction[J]. J Vasc Access, 2020, 21(4): 520-523. doi:10.1177/1129729819890472.
pmid: 31774035 |
| [4] |
Al-Jaishi AA, Liu AR, Lok CE, et al. Complications of the arteriovenous fistula: A systematic review[J]. J Am Soc Nephrol, 2017, 28(6):1839-1850. doi:10.1681/ASN.2016040412.
pmid: 28031406 |
| [5] | Staaf K, Fernström A, Uhlin F. Cannulation technique and complications in arteriovenous fistulas:A swedish renal registry-based cohort study[J]. BMC Nephrol, 2021, 22(1):256. doi:10.1186/s12882-021-02458-z. |
| [6] | McCoy IE, Shieh L, Fatehi P. Reducing phlebotomy in hemodialysis patients: A quality improvement study[J]. Kidney Med, 2020, 2(4):432-436. doi:10.1016/j.xkme.2020.05.006. |
| [7] | Ten Berge MG, Yo TI, Kerver A, et al. Perforating veins: An anatomical approach to arteriovenous fistula performance in the forearm[J]. Eur J Vasc Endovasc Surg, 2011, 42(1):103-106. doi:10.1016/j.ejvs.2011.03.008. |
| [8] | Norton de Matos A, Sousa CN, Almeida P, et al. Radiocephalic fistula recovery using the brachial vein and forearm basilic vein: A case series and literature review[J]. Ther Apher Dial, 2018, 22(6):570-574. doi:10.1111/1744-9987.12719. |
| [9] | Mendes D, Almeida P, Pinelo A, et al. Antecubital perforating vein stent-grafting for radiocephalic arteriovenous fistula recovery: A case report[J]. Semin Dial, 2023, 36(4):348-351. doi:10.1111/sdi.13158. |
| [10] | Turmel-Rodrigues L, Pengloan J, Baudin S, et al. Treatment of stenosis and thrombosis in haemodialysis fistulas and grafts by interventional radiology[J]. Nephrol Dial Transplant, 2000, 15(12):2029-2036. doi:10.1093/ndt/15.12.2029. |
| [11] |
Turmel-Rodrigues L. Dilatation is usually the best treatment for stenosis of the arteriovenous hemodialysis fistula[J]. Nat Clin Pract Nephrol, 2008, 4(3):116-117. doi:10.1038/ncpneph0711.
pmid: 18212783 |
| [12] | Peregrin JH, Rocek M. Results of a peripheral cutting balloon prospective multicenter European registry in hemodialysis vascular access[J]. Cardiovasc Intervent Radiol, 2007, 30(2):212-215. doi:10.1007/s00270-006-0020-0. |
| [13] |
Pirozzi N, Scrivano J, Pettorini L, et al. Preventive hemostasis for hemodialysis vascular access surgical reinterventions[J]. J Vasc Access, 2013, 14(2):193-195. doi:10.5301/jva.5000104.
pmid: 23032956 |
| [14] |
Ravani P, Palmer SC, Oliver MJ, et al. Associations between hemodialysis access type and clinical outcomes: A systematic review[J]. J Am Soc Nephrol, 2013, 24(3):465-473. doi:10.1681/ASN.2012070643.
pmid: 23431075 |
| [15] | Mendes D, Almeida P, Sousa C, et al. Outflow rescue of elbow-blockade forearm arteriovenous fistulas: Outcomes of open surgical techniques[J]. Ann Vasc Surg, 2023, 94:280-288. doi:10.1016/j.avsg.2023.02.028. |
| [16] |
Wang Z, Hong Y, Wei Z, et al. Managing thrombosis of arteriovenous fistula accompanied by aneurysm and single outflow of elbow perforating vein: A case report[J]. BMC Nephrol, 2022, 23(1):271. doi:10.1186/s12882-022-02897-2.
pmid: 35907795 |
| [17] | 中国医院协会血液净化中心分会血管通路工作组. 中国血液透析用血管通路专家共识(第 2 版)[J]. 中国血液净化, 2019, 18(6): 365-381. doi:10.3969/j.issn.1671-4091.2019.06.001. |
| [18] | Lok CE, Huber TS, Lee T, et al. KDOQI clinical practice guideline for vascular access: 2019 update[J]. Am J Kidney Dis, 2020, 75(4Suppl 2): S1-S164. doi:10.1053/j.ajkd.2019.12.001. |
| [19] |
Caro Acevedo P, Marchante R, Thuissard IJ, et al. A systematic follow-up protocol achieving a low hemodialysis graft thrombosis rate[J]. J Vasc Access, 2019, 20(6):683-690. doi:10.1177/1129729819838795.
pmid: 31002279 |
| [20] | 刘文静, 王宇飞, 张倍豪, 等. 移植物动静脉内瘘血栓形成的流行病学特征、干预效果及影响因素分析[J]. 中华肾脏病杂志, 2024, 40(7): 526-532. doi: 10.3760/cma.j.cn441217-20231218-01230. |
| [21] | 彭嘉欣, 万恒. 131例人工血管移植物内瘘中期随访结果[J]. 中华普通外科杂志, 2021, 36(4): 286-289. doi:10.3760/cma.j.cn113855-20200317-00213. |
| [22] |
Fumagalli G, Trovato F, Migliori M, et al. The forearm arteriovenous graft between the brachial artery and the brachial vein as a reliable dialysis vascular access for patients with inadequate superficial veins[J]. J Vasc Surg, 2019, 70(1): 199-207.e4. doi:10.1016/j.jvs.2018.10.101.
pmid: 30894304 |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||